Step-By-Step Guide to Health Insurance Claims for International Students in the U.S.

The last stop for international students after their overseas medical treatment – claim – is often the most unfamiliar step for students due to the huge difference in medical treatment in the United States.
According to Student Medicover’s professional customer service team, questions related to insurance claims have been the most frequently asked questions by students, such as how should I use my insurance to make a claim? How long do I have to wait? How can I check the progress of my claim?
In this article, we will help you master the basic knowledge of a claim, and you will never have a problem in making a claim in the U.S.!
Navigation
What are health insurance claims?
The health insurance claim is a request for your insurance company to pay for the medical treatment your insurance covers.
You can skip the claim process by visiting an in-network hospital or doctor. Medical care institutions will contact and send your claim to UnitedHealthcare StudentResource directly. Remember to bring your insurance ID card for your appointment.
What are the most common health insurance claims in the U.S.?
- Direct Billing : Bring your insurance card so you don’t have to make your own claims
In most cases, if the hospital you visit is a School Hospital or in-network provider, most school hospitals and in-network hospitals will send your bill directly to the insurance company, as long as you present your insurance card prior to your visit, eliminating the complicated process of paying the bill first and then settling the claim.
- Reimbursement Claim: Request to pay the bill yourself first then file the claim
If you go to an out-of-network provider or the School’s Health Center, most providers will need you to pay the medical bills and then file a claim with the insurance company.
How to file a claim at an out-of-network hospital?
Step1 Prepare the claim package
*All of the following documents need to be provided in PDF format
Medical claim/Foreign claim
a. Itemized Bills
An itemized bill is a list of bills. You can obtain this from your provider whether you see a doctor on-campus or off-campus. A valid Itemized bill contains the name, address, phone number, and Taxpayer ID of the provider, Procedure Code, Diagnosis Code, the date of service, and charge amount.
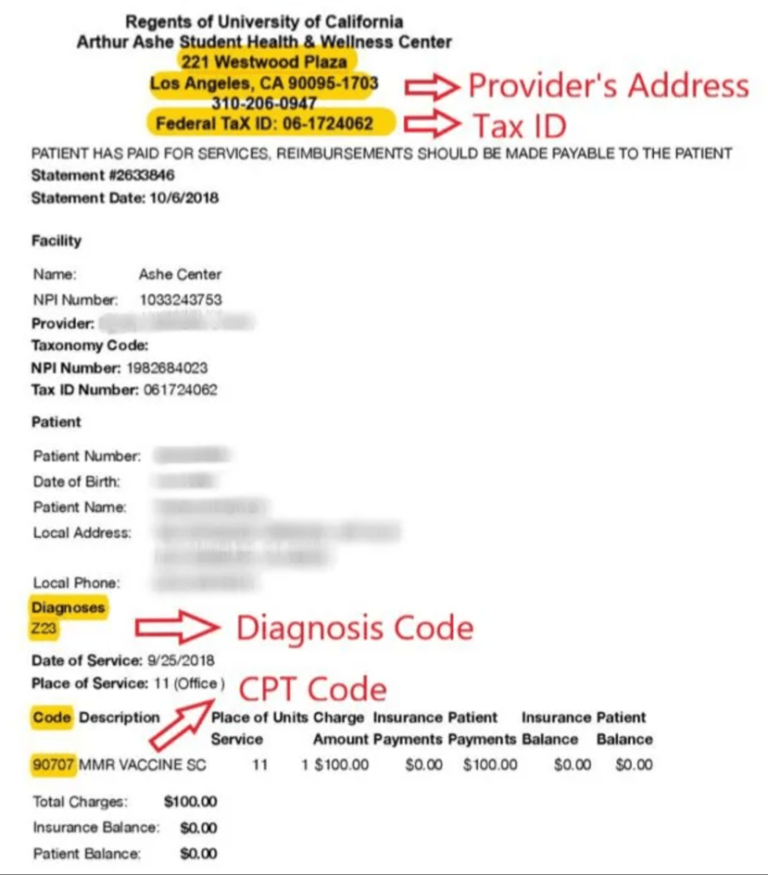
b. Proof of Payment
A medical bill is a list of charges issued by the provider of the visit. Evidence that shows you have already paid for the medical care service.
Notice: required documents may vary slightly for different payment methods.
▻ Credit Card Payments
If you paid by credit card, you will need to provide a credit card statement showing the full name of the cardholder, the name of the institution and payment information for each date of service.
▻ ATM or Debit Card Payments
A bank statement showing the full name of the account holder, the name of the institution and payment information for each date of service is required.
▻ Cash Payments
If paying by cash, students are required to retain the receipt and UHCSR will call the service provider to verify.
Prescription claim
- Copy of insurance card
- Prescription form: contains patient’s name, physician’s name, name of the medication, date dispensed, quantity, and purchase price
- Proof of payment (same requirements as above)
Step2 Claims Submission
Log in to the insurance company’s webpage and submit your documents.
For example, if you have Student Medicover insurance, you can log in to your UHCSR account, select submit claim, fill out the claim information, and then upload the documents according to the type of claim.
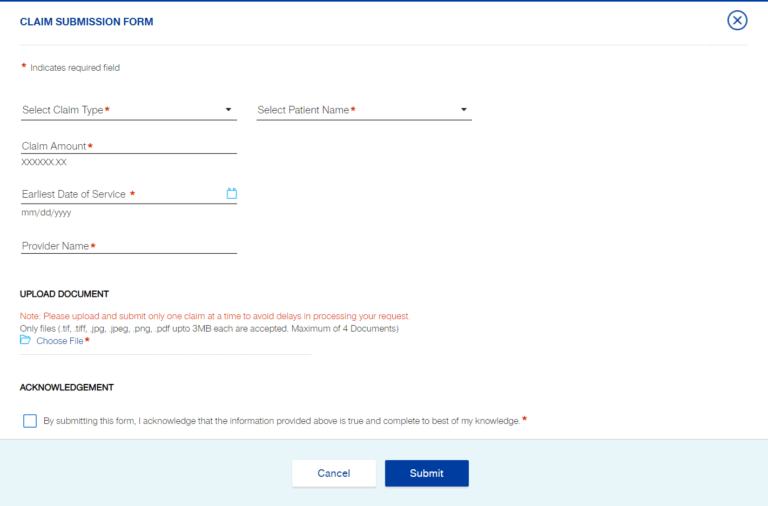
*Students can also email, mail, fax or send the above documents directly to the appropriate insurance company.
For example, if you have Student Medicover insurance, simply send the documents to UnitedHealthcare StudentResources at
Email:[email protected]
Mailing address: UnitedHealthcare Student Resources, P.O. Box 809025, Dallas, TX 75380-9025
Fax:469-229-5625
Step3 Waiting for claims
When the students submit the claim documents, the claim is completed, the next is to wait for the insurance company to complete the claim, the insurance company claims process and the estimated time is as follows:
View Claims Progress
(10-20 business days)
Supplementary documents
(10-20 business days)
View EOB file
(3-5 business days)
Receiving checks
(10-20 business days)
Several Types of Claim status
- receive
- pending(Begin processing not yet completed)
- complete + EOB pending(Processing is complete but the EOB is still pending)
- complete
>>Usually, you can find the claim status after 20 business days, and you can find it in your UHCSR account if you have Student Medicover insurance. If your claim status is still pending for more than 20 days, please check the claim letter in “my claim” in your UHCSR account to see if there is any additional information that needs to be submitted.
>When your claim status shows complete, check in my claim in your UHCSR account and click on view “More Options” to download the EOB. If you can’t click on it, just change your browser or turn off the blocking feature.
Step4 Check out the EOB
The EOB is called Explain of Benefits, and is a document that is generated when the insurance company has processed the claim. Students should not rush to pay after receiving it, unlike the official bill, the EOB is only a statement explaining the insurance benefits.
After that, you will receive a bill from the hospital, which is the bill that you need to pay, but please make sure to check if the amount shown on the bill is the same as the amount on the EOB before you pay.
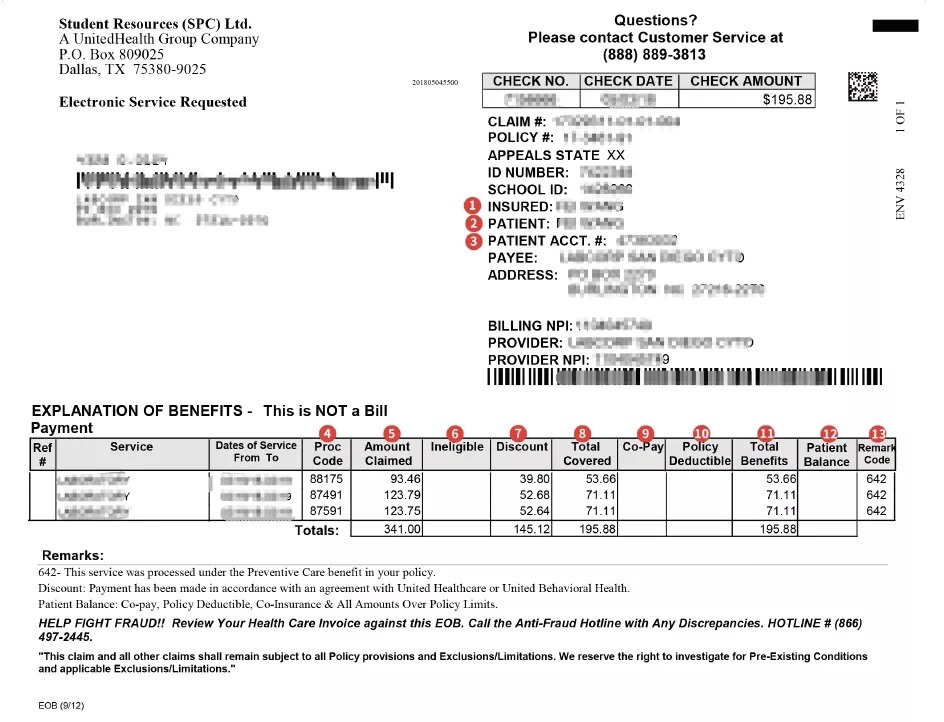

- Insured:Insured person
- Patient: Patient
- Patient Account Number: Patient account information
- Procedure code: Medical procedure code that provides accurate descriptive language for medical, surgical, and diagnostic purposes
- Amount Claim: The total amount of claims submitted to the insurance company by the physician/hospital
- Ineligible: the cost of services/treatment not covered by insurance
- Discount: discount for in-network hospitals
- Total covered: the total amount of insurance claims
- Co-pay: the amount you have to pay for each visit, similar to an office visit
- Policy deductible: The amount you have to pay out of pocket before your insurance company will pay for your medical expenses. It accumulates over the academic year and you do not have to pay it after you reach it.
- Total benefits: The actual cost paid by the insurance
- Patient Balance: The amount the insured will pay
- Remark Code: The code used for the description in the Remark area (Optional)
Step5 Get the advance payment back
Usually, the insurance company will send the check amount to the student in the mail, which takes about 2 weeks.
If you do not receive the check amount within a month, you will need to contact the insurance company yourself. If you have SM insurance, you can call UHCSR Customer Service at 866-352-8632 (Student Medicover customer line) to reissue a check for your claim. It is important to note that checks need to be redeemed within 60 days.
YOU MAY ALSO ENJOY THESE ARTICLES:

